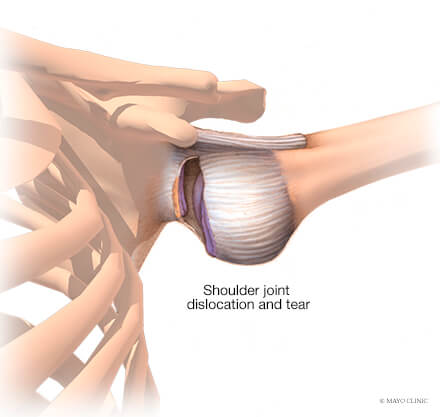
The shoulder is a “ball and socket” joint that is comprised of the humeral head (the “ball”) and the glenoid (“socket”). The humeral head is the top part of the upper arm bone (humerus) while the glenoid is a very shallow socket located on the shoulder blade (scapula). The term “shoulder instability” is used to describe what happens when the humeral head separates from the glenoid. This can be a very quick partial separation that lasts only a few seconds (subluxation), or it can be a more significant condition where the ball and socket get stuck in the dislocated position.
When a shoulder instability event occurs, it can also cause other damage to the shoulder such as tears of the labrum (rim of soft cartilage tissue around the glenoid), cartilage injuries, rotator cuff tears, or even fractures. Shoulder instability can occur following a traumatic accident such as a fall or collision with another athlete or object. It can also occur without significant trauma or injury, and this type of shoulder instability is more common in people who are exceptionally flexible with “loose” joints or connective tissue problems such as Ehlers Danlos.


